Current Issue: June 2026
Editor's Choice
This month's highlight articles
Table of Contents
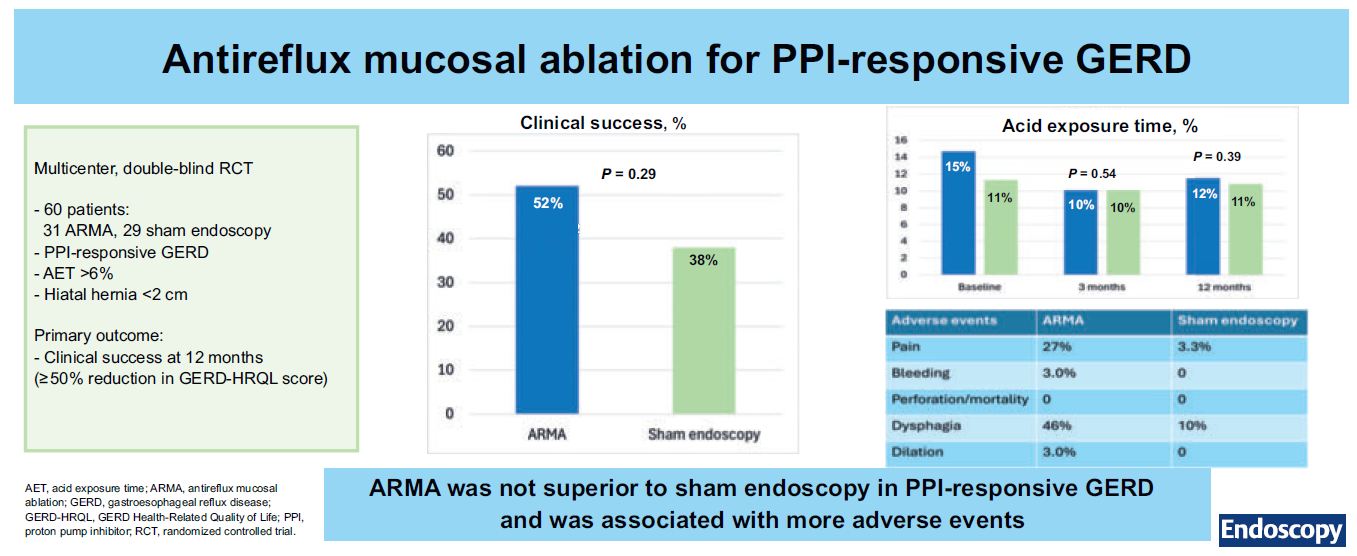
Original article
Original article
Original article
Editorial
Original article
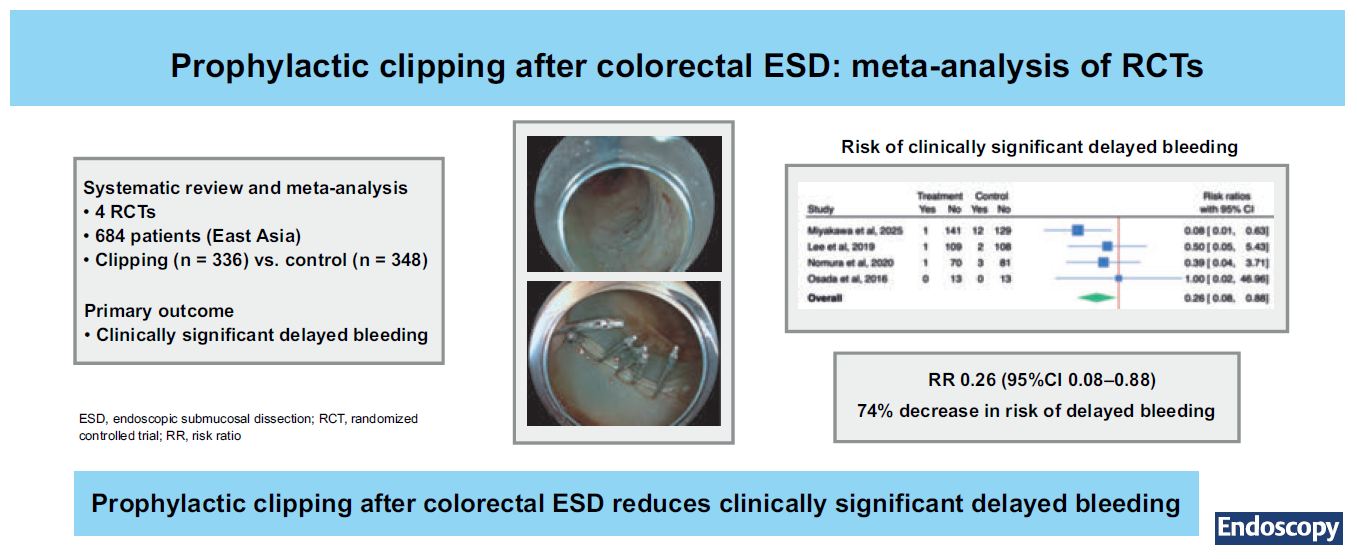
Systematic review
Systematic review
Innovations and brief communications
Innovations and brief communications
Innovations and brief communications
E-Videos
Letter to the editor
Letter to the editor
In this issue
Newsletter
Don't want to miss important information?
Sign up for your monthly Endoscopy-Newsletter: Our Editorial Team offers insight in what's new and important.